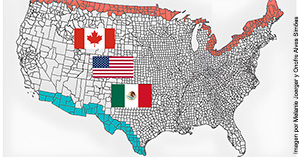
Mortalidad a nivel de condado en las regiones fronterizas Estados Unidos-México y Estados Unidos-Canadá
Mortality at the county level in the USA-Mexico and USA-Canada border regions
https://doi.org/10.21670/ref.2402138
Palabras clave:
mortalidad por condado, frontera entre EUA y México, frontera entre EUA y Canadá, paradoja hispana, índicesResumen
Las áreas cercanas a la frontera de un país tienen una demografía interesante ya que son las zonas donde chocan dos culturas. Estados Unidos tiene dos largas fronteras terrestres con Canadá y México. Se examina la mortalidad entre 1999 y 2019 a nivel de condado en las dos regiones fronterizas, en comparación con las regiones no fronterizas de los estados fronterizos. El análisis se basa en índices, con combinaciones de factores como edad, sexo y causa de muerte. Los resultados confirman diferencias entre regiones fronterizas y no fronterizas y entre fronteras. Hasta donde se sabe, no existe un estudio previo de mortalidad en ambas fronteras y así la contribución del trabajo es demostrar las diferencias entre las regiones fronterizas y no fronterizas para las dos fronteras y discutir las posibles razones. El análisis más detallado a nivel de condado, incluso con ciertas limitaciones de datos, brinda información importante sobre el tema.Abstract The areas near a country border have interesting demographics since they are the zones where two cultures collide. The USA has two long land borders with Canada and Mexico. Mortality between 1999-2019 is examined at the county level in the two border regions, compared to the non-border regions of the border states. Analysis is based on single figure indices, with combinations of confounders age, gender and cause of death. Findings confirm differences between border and non-border regions, with opposite results at each border. As far as is known there is no previous mortality study concerning both borders and therefore the contribution of the work is to demonstrate the differences between the border and non-border regions for the two borders and discuss possible reasons. Further, we show that the more detailed analysis at the county level, even with certain data limitations, gives important insights to the topic.
Citas
Abraído-Lanza, A. F., Dohrenwend, B. P., Ng-Mak, D. S. & Turner, J. B. (1999). The Latino mortality paradox: a test of the “salmon bias” and healthy migrant hypotheses. American Journal of Public Health, 89(10), 1543-1548. https://doi.org/10.2105/AJPH.89.10.1543 DOI: https://doi.org/10.2105/AJPH.89.10.1543
Adler, N. E., Boyce, T., Chesney, M. A., Cohen, S., Folkman, S., Kahn, R. L. & Syme, S. L. (1994). Socioeconomic status and health: the challenge of the gradient. American Psychologist, 49(1), 15-24. https://doi.org/10.1037//0003-066x.49.1.15 DOI: https://doi.org/10.1037/0003-066X.49.1.15
Anderson, B. (n. d.). The border and the Ontario economy. Cross-Border Transportation Centre-University of Windsor. http://cbinstitute.ca/wp-content/uploads/2015/09/The-Border-and-the-Ontario-Economy.pdf
Band, P. R., Zielinski, J. M., Jiang, H. & Liu, L. (2006). Canada-US border air quality strategy (BAQS): preliminary results of mortality and cancer incidence in Windsor, Canada. WIT Transactions on Ecology and the Environment, 86, 777-783. https://www.witpress.com/Secure/elibrary/papers/AIR06/AIR06076FU1.pdf DOI: https://doi.org/10.2495/AIR06076
Banegas, M. P., Bird, Y., Moraros, J., King, S., Prapsiri, S. & Thompson, B. (2012). Breast cancer knowledge, attitudes, and early detection practices in United States-Mexico border Latinas. Journal of Women’s Health, 21(1), 101-107. https://doi.org/10.1089/jwh.2010.2638 DOI: https://doi.org/10.1089/jwh.2010.2638
Becker, T. M., Wiggins, C., Key, C. R. & Samet, J. M. (1988). Ischemic heart disease mortality in Hispanics, American Indians, and non-Hispanic whites in New Mexico, 1958-1982. Circulation, 78(2), 302-309. https://doi.org/10.1161/01.cir.78.2.302 DOI: https://doi.org/10.1161/01.CIR.78.2.302
Breslow, N. E. & Day, N. E. (1987). Statistical methods in cancer research. Volume II-The design and analysis of cohort studies (IARC Scientific Publications No. 82). International Agency for Research on Cancer. https://publications.iarc.fr/Book-And-Report-Series/Iarc-Scientific-Publications/Statistical-Methods-In-Cancer-Research-Volume-II-The-Design-And-Analysis-Of-Cohort-Studies-1986
Bureau of Transportation Statistics. (n. d.). US-Canada ports of entry. U.S. Department of Transportation. Retrieved on August 7, 2023 from https //data.bts.gov/Research-and-Statistics/US-Canada-Ports-of-Entry/s8z8-5vi3
Centers for Disease Control and Prevention. (n. d.). About multiple cause of death with U.S.-Mexico border regions, 1999-2020. CDC WONDER Online Database. Retrieved on August 7, 2023 from http //wonder.cdc.gov/ucd-border.html
Crimmins, E. M., Kim, J. K. & Seeman, T. E. (2009). Poverty and biological risk: the earlier “aging” of the poor. The Journals of Gerontology Series A: Biological Sciences and Medical Sciences, 64A(2), 286-292. https://doi.org/10.1093/gerona/gln010 DOI: https://doi.org/10.1093/gerona/gln010
Díaz-Apodaca, B. A., Ebrahim, S., McCormack, V., De Cosío, F. G. & Ruiz-Holguín, R. (2010). Prevalence of type 2 diabetes and impaired fasting glucose: cross-sectional study of multiethnic adult population at the United States-Mexico border. Revista Panamericana de Salud Pública, 28(3), 174-181. https://iris.paho.org/handle/10665.2/9638?locale-attribute=en DOI: https://doi.org/10.1590/S1020-49892010000900007
Dwyer-Lindgren, L., Bertozzi-Villa, A., Stubbs, R. W., Morozoff, C., Kutz, M. J., Huynh, C., Barber, R. M., Shackelford, K. A., Mackenbach, J. P., Van Lenthe, F. J., Flaxman, A. D., Naghavi, M., Mokdad, A. H. & Murray, C. J. L. (2016). US county-level trends in mortality rates for major causes of death, 1980-2014. JAMA, 316(22), 2385-2401. https://doi.org/10.1001/jama.2016.13645 DOI: https://doi.org/10.1001/jama.2016.13645
Eschbach, K., Ostir, G. V., Patel, K. V., Markides, K. S. & Goodwin, J. S. (2004). Neighborhood context and mortality among older Mexican Americans: Is there a barrio advantage? American Journal of Public Health, 94(10), 1807-1812. https://doi.org/10.2105/AJPH.94.10.1807 DOI: https://doi.org/10.2105/AJPH.94.10.1807
Feeny, D., Kaplan, M. S., Huguet, N. & McFarland, B. H. (2010). Comparing population health in the United States and Canada. Population Health Metrics, 8, Article 8. https://doi.org/10.1186/1478-7954-8-8 DOI: https://doi.org/10.1186/1478-7954-8-8
Fuller-Thomson, E., Brennenstuhl, S., Cooper, R. & Kuh, D. (2015). An investigation of the healthy migrant hypothesis: Pre-emigration characteristics of those in the British 1946 birth cohort study. Canadian Journal of Public Health/Revue Canadienne de Santé Publique, 106(8), e502-e508. https://doi.org/10.17269/CJPH.106.5218 DOI: https://doi.org/10.17269/CJPH.106.5218
Herrera, D. G., Schiefelbein, E. L., Smith, R., Rojas, R., Mirchandani, G. G. & McDonald, J. A. (2012). Cervical cancer screening in the US-Mexico border region: a binational analysis. Maternal and Child Health Journal, 16(2), 298-306. https://doi.org/10.1007/s10995-012-1130-8 DOI: https://doi.org/10.1007/s10995-012-1130-8
Hummer, R. A., Powers, D. A., Pullum, S. G., Gossman, G. L. & Frisbie, W. P. (2007). Paradox found (again): infant mortality among the Mexican-origin population in the United States. Demography, 44(3), 441-457. https://doi.org/10.1353/dem.2007.0028 DOI: https://doi.org/10.1353/dem.2007.0028
Hummer, R. A., Rogers, R. G., Amir, S. H., Forbes, D. & Frisbie, W. P. (2000). Adult mortality differentials among Hispanic subgroups and non-Hispanic whites. Social Science Quarterly, 81(1), 459-476. https://www.jstor.org/stable/42864393
Israel, E. & Batalova, J. (2020, November 5). Mexican immigrants in the United States. Migration Policy Institute. https //www.migrationpolicy.org/article/mexican-immigrants-united-states-2019
Israel, E. & Batalova, J. (2021, June 15). Canadian immigrants in the United States. Migration Policy Institute. https //www.migrationpolicy.org/article/canadian-immigrants-united-states-2021#distribution
James, W., Cossman, J. & Wolf, J. K. (2018). Persistence of death in the United States: the remarkably different mortality patterns between America’s Heartland and Dixieland. Demographic Research, 39, Article 33, 897-910. https://doi.org/10.4054/DemRes.2018.39.33 DOI: https://doi.org/10.4054/DemRes.2018.39.33
Kim, I., Lim, H.-K., Kang, H.-Y. & Khang, Y.-H. (2020). Comparison of three small-area mortality metrics according to urbanity in Korea: the standardized mortality ratio, comparative mortality figure, and life expectancy. Population Health Metrics, 18, Article 3. https://doi.org/10.1186/s12963-020-00210-7 DOI: https://doi.org/10.1186/s12963-020-00210-7
Kolčić, I. & Polašek, O. (2009). Healthy migrant effect within Croatia. Collegium antropologicum, 33(1), 141-145. https://pubmed.ncbi.nlm.nih.gov/19563160/
Krueger, P. M., Bhaloo, T. & Rosenau, P. V. (2009). Health lifestyles in the United States and Canada: Are we really so different? Social Science Quarterly, 90(5), 1380-1402. https://doi.org/10.1111/j.1540-6237.2009.00660.x DOI: https://doi.org/10.1111/j.1540-6237.2009.00660.x
Kumar, D. & Klefsjö, B. (1994). Proportional hazards model: a review. Reliability Engineering & System Safety, 44(2), 177-188. https://doi.org/10.1016/0951-8320(94)90010-8 DOI: https://doi.org/10.1016/0951-8320(94)90010-8
Liao, Y., Cooper, R. S., Cao, G., Durazo-Arvizu, R., Kaufman, J. S., Luke, A. & McGee, D. L. (1998). Mortality patterns among adult Hispanics: findings from the NHIS, 1986 to 1990. American Journal of Public Health, 88(2), 227-232. https://doi.org/10.2105/AJPH.88.2.227 DOI: https://doi.org/10.2105/AJPH.88.2.227
Lu, Y. & Qin L. (2014). Healthy migrant and salmon bias hypotheses: a study of health and internal migration in China. Social Science and Medicine, 102, 41-48. https://doi.org/10.1016/j.socscimed.2013.11.040 DOI: https://doi.org/10.1016/j.socscimed.2013.11.040
Markides, K. S. & Coreil, J. (1986). The health of Hispanics in the southwestern United States an epidemiologic paradox. Public Health Reports, 101(3), 253-265. https://pubmed.ncbi.nlm.nih.gov/3086917/
McDonald, J. A. & Paulozzi, L. J. (2019, April). Parsing the paradox: hispanic mortality in the US by detailed cause of death. Journal of Immigrant and Minority Health, 21(2), 237-245. https://doi.org/10.1007/s10903-018-0737-2 DOI: https://doi.org/10.1007/s10903-018-0737-2
Mills, B. A. & Caetano, R. (2016). Alcohol use and related problems along the United States-Mexico border. Alcohol Research: Current Reviews, 38(1), 79-81. https://pubmed.ncbi.nlm.nih.gov/27159814/
Moya, E. M., Chávez-Baray, S. M., Wood, W. W. & Martinez, O. (2016). Nuestra casa: an advocacy initiative to reduce inequalities and tuberculosis along the US-Mexico border. International Public Health Journal, 8(2), 107-119. http://www.ncbi.nlm.nih.gov/pmc/articles/pmc6150456/
Ontario Ministry of Economic Development, Job Creation and Trade. (2021). Ontario and Michigan partnering on cross-border transportation technologies. Government of Ontario. https://news.ontario.ca/en/release/1000752/ontario-and-michiganpartnering-on-cross-border-transportation-technologies
Orraca Romano, P. P. (2015). Immigrants and cross-border workers in the U.S.-Mexico border region. Frontera Norte, 27(53), 5-34. https://doi.org/10.17428/rfn.v27i53.97
Oyana, T. J., Rogerson, P. & Lwebuga-Mukasa, J. S. (2004). Geographic clustering of adult asthma hospitalization and residential exposure to pollution at a United States-Canada border crossing. American Journal of Public Health, 94(7), 1250-1257. https://doi.org/10.2105/AJPH.94.7.1250 DOI: https://doi.org/10.2105/AJPH.94.7.1250
Palloni, A. & Arias, E. (2004). Paradox lost: explaining the hispanic adult mortality advantage. Demography, 41(3), 385-415. https://doi.org/10.1353/dem.2004.0024 DOI: https://doi.org/10.1353/dem.2004.0024
Pew Research Center. (2023). Data and Resources. https://www.pewresearch.org/hispanic/data-and-resources/
Ruiz, J. M., Hamann, H. A., Mehl, M. R. & O’Connor, M-F. (2016). The Hispanic health paradox: from epidemiological phenomenon to contribution opportunities for psychological science. Group Processes & Intergroup Relations, 19(4), 462-476. https://doi.org/10.1177/1368430216638540 DOI: https://doi.org/10.1177/1368430216638540
Salinas, J. J., Su, D. & Al Snih, S. (2013). Border health in the shadow of the Hispanic paradox issues in the conceptualization of health disparities in older Mexican Americans living in the Southwest. Journal of Cross-Cultural Gerontology, 28(3), 251-266. https://doi.org/10.1007/s10823-013-9202-9 DOI: https://doi.org/10.1007/s10823-013-9202-9
Schoenbach, V. J. & Rosamond, W. D. (2000). Understanding fundamentals of epidemiology. An evolving text. University of North Carolina at Chapel Hill. http //www.epidemiolog.net/evolving/FundamentalsOfEpidemiology.pdf
Shai, D. & Rosenwaike, I. (1987). Mortality among Hispanics in metropolitan Chicago: an examination based on vital statistics data. Journal of Chronic Diseases, 40(5), 445-451. https://doi.org/10.1016/0021-9681(87)90178-0 DOI: https://doi.org/10.1016/0021-9681(87)90178-0
Sheps, M. C. (1966). On the person years concept in Epidemiology and Demography. The Milbank Memorial Fund Quarterly, 44(1), 69-91. https://doi.org/10.2307/3349039 DOI: https://doi.org/10.2307/3349039
Siddiqi, A. & Hertzman, C. (2007). Towards an epidemiological understanding of the effects of long-term institutional changes on population health: a case study of Canada versus the USA. Social Science & Medicine, 64(3), 589-603. https://doi.org/10.1016/j.socscimed.2006.09.034 DOI: https://doi.org/10.1016/j.socscimed.2006.09.034
Sorlie, P. D., Backlund, E., Johnson, N. J. & Rogot, E. (1993). Mortality by Hispanic status in the United States. JAMA, 270(20), 2464-2468. https://jamanetwork.com/journals/jama/article-abstract/409364 DOI: https://doi.org/10.1001/jama.270.20.2464
Sorlie, P. D., Backlund, E. & Keller, J. B. (1995). US mortality by economic, demographic, and social characteristics: the National Longitudinal Mortality Study. American Journal of Public Health, 85(7), 949-956. https://ajph.aphapublications.org/doi/pdf/10.2105/AJPH.85.7.949 DOI: https://doi.org/10.2105/AJPH.85.7.949
Stoddard, P., He, G., Vijayaraghavan, M. & Schillinger, D. (2010). Disparities in undiagnosed diabetes among United States-Mexico border populations. Revista Panamericana de Salud Pública, 28(3), 198-206. https://iris.paho.org/handle/10665.2/9634?locale-attribute=en DOI: https://doi.org/10.1590/S1020-49892010000900010
United States-Mexico Border Health Commission. (2020). Healthy border 2020: a prevention & health promotion initiative. US Department of Health and Human Services. https //www.hhs.gov/sites/default/files/res_2805.pdf